DiagnosticInformatics Approaches Computational prediction of heart failure
In the current era of technology and innovation, terms such as “digital health” and “machine-learning” feature in medicine more and more frequently, and with good reason. Computational models enable researchers to peel back the layers of complexity of the human body, helping visualise and understand organ functions, and now this tool may be used to monitor disease progression, tailor treatments and predict patients’ outcome.
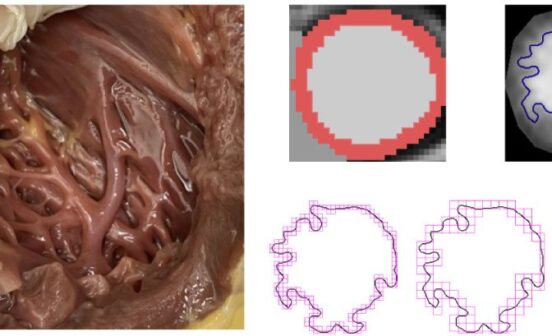
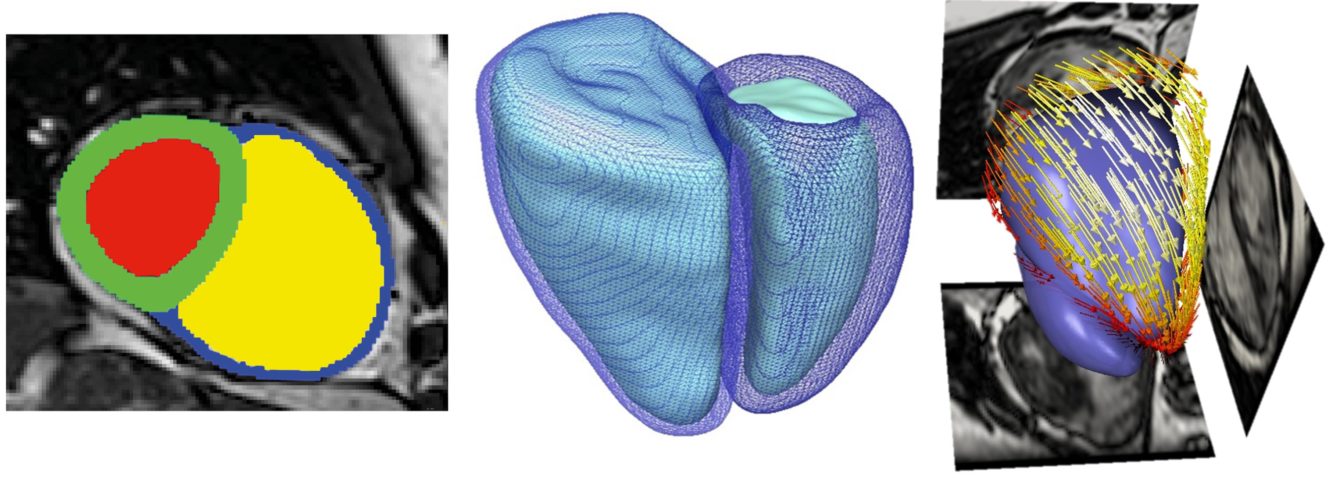
Researchers from the NIHR Imperial Biomedical Research Centre (BRC) have developed a software algorithm that learns from 3D patterns of a contracting heart, thereby accurately predicting when the heart may stop in patients with pulmonary hypertension. The latter is characterised by the thickening of the walls of arteries that supply the lungs from the right-hand side of the heart. This condition may affect people of any age, but particularly those with pre-existing heart or lung conditions.
Dr. Declan O’Regan and colleagues at Hammersmith Hospital recorded heart shape changes from 256 patients with pulmonary hypertension using MRI at each heartbeat. The software analysed patterns of heart movement, and patients with reduced contractions in specific right-side regions of the heart were predicted to have poor prognosis. The rate of successful one-year survival prediction was approximately 80%, with a potential predictive power of five years into the future of each patient.
This study was published in Radiology and was co-funded by the NIHR Imperial BRC. It is an excellent example of extending the potential of existing imaging resources via applying computational analyses. In addition to accurate disease risk prediction, these artificial intelligence (AI) models can help clinicians tailor their treatments to better suit individual patients, without the need for invasive procedures. Further developments are currently underway to increase the depth of cardiac 3D modelling, as well as extend this approach to other heart conditions.