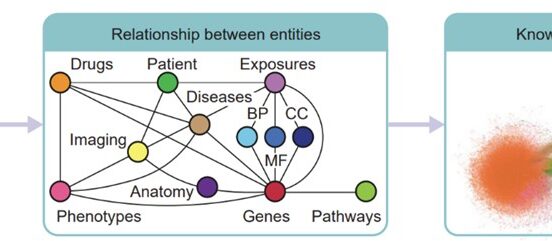
Our work in Digital Health aims to drive improvements in the quality, safety and experience of healthcare using data-driven insights, and co-designed digital interventions and technologies. Through data analytics (including machine learning and artificial intelligence), new software development/integration, and rigorous testing and evaluation, we are translating digital interventions into improvements in healthcare delivery for clinicians, patients and the public.
Why this Research is Needed
Communities in north Westminster, north Kensington, and south Brent are amongst the 20% most deprived areas in the country, with significant health outcome disparities and an 18-year life expectancy gap between the most and least deprived. Alongside these public health challenges, the pandemic has increased the demand for innovative digital solutions that can enhance the resilience of the healthcare system and support patient engagement. Our research is responding to these challenges by generating data-driven insights and digital solutions to address the most pressing health priorities and inequalities – for example, in diabetes, mental health, and multi-morbidity.
Theme Aims
Three programmes of research aim to improve healthcare delivery using digital innovation and AI technologies:
- The Translational Data Analytics workstream brings together information across different electronic health record systems to provide clinical decision support to front-line healthcare staff – ensuring they have the right information, in the right place, at the right time. Robust evaluation of our innovative decision support tools will include assessing the impacts on clinician behaviours, productivity metrics, patient experience, health inequalities, and clinical outcomes.
- The AI Testbed for Digital Health programme will create the digital research infrastructure for safe, effective and ethical adoption of AI-driven technologies in health and social care. We will apply AI to image and omics data in routine care for early diagnosis and precision medicine, and develop new-generation Interpretable AI technologies that are understood and trusted by patients and clinicians.
- The Real-World Evidence workstream aims to develop new approaches to increasing the efficiency of clinical trials and improving recruitment in under-represented population groups. De-identified routinely-collected data, captured during the patient journey through the health system, will enable us to evaluate real-world adoption of interventions to inform complex healthcare delivery problems.
Upcoming /Ongoing Projects within the Theme
Inclusive Recruitment
Diverse NHS staff are essential to the delivery of high-quality and person-centred services, however, the COVID-19 pandemic has shown that Black and Minority Ethnic (BME) staff have very different and unequal experiences of the NHS as a workplace, with less representation in more senior roles. To address this, Imperial College Healthcare NHS Trust has implemented an inclusive recruitment programme which includes mandatory diverse interview panels and requires all hiring managers to write a letter to the Trust Chief Executive Officer (CEO) to justify their chosen candidate. Working with the Trust’s workforce team, we are using advanced analytics and natural language processing to analyse routine recruitment data and the Letters to the CEO, providing real-time insights into the effectiveness of this inclusive recruitment programme to support the Trust in achieving its EDI objectives.
Falls
Every day the NHS spends around £6 million on falls; falls occurring in hospitals account for 25% of this expenditure. The human cost of falls ranges from distress and loss of confidence to head injuries, bone fractures, and even death. Our research will use routine data from electronic patient records and incident reporting systems to better understand why patients fall in hospitals, with a particular emphasis on under-represented groups (e.g. patients with English as a second language). We will develop and evaluate an integrated informatics platform that applies Natural Language Processing to falls documentation to provide semi-automated, near-real-time reports to Imperial College Healthcare NHS Trust for coordinated safety monitoring and improvement.
Clinical Decision Support in Ovarian Cancer
Ovarian cancer is a devastating disease with most patients presenting at an advanced, incurable stage. There is a wealth of data held across NHS systems that could help improve outcomes for such patients but it is often written in clinical notes across the electronic health record, and not held in a single location. This makes finding all the relevant information quickly challenging, with the potential for some aspects to be missed.
Our team of healthcare professionals, researchers, and data scientists have built a new system using advanced text analysis called natural language processing bringing important and relevant clinical facts together into a single location such that it can be easily accessed by the multi-disciplinary cancer team. We are now evaluating the impact of the system on delivering benefits for patients and their outcomes, improving data quality, and saving money through improved processes and time savings.
Increasing real-world clinical trial capacity
The use of electronic health records (EHRs) can support the conduct of randomised clinical trials (RCTs) in conditions closer to usual clinical practice. This project will expand consultation with patients and citizens on the acceptable use of their healthcare records for clinical trials within a safe and secure data environment and deploy clinical trial technologies for the design, recruitment, and conduct of studies embedded within digital primary and secondary care clinical records.
Real World follow-up of interventions
The project aims to use linked healthcare data and additional regional/national data sources to supplement clinical trial data to provide evidence of effectiveness in interventions where good data are lacking. The goal is to understand health and digital inequalities, unintended consequences, and the holistic impact of healthcare interventions by taking a population approach. One exemplar project will evaluate the impact of a digital intervention for a mental health condition on adverse events and improved outcomes for a patient group in the community.
Optimising health and social care systems
This project aims to use integrated machine learning and optimisation approaches to improve the delivery of high-quality, safe care and reduce inequalities for patients in North West London. The project will focus on analysing patient journeys through the health and social care system, characterising delays and inequalities, and developing an open-source framework to optimise pathways based on routinely collected integrated health data.
Patient and Public Involvement, Engagement and Participation
The theme has recruited four community partners that are all members of the public currently living and/or studying in Northwest London. These community partners will be actively involved in providing strategic input into the theme’s activities and meaningfully connecting researchers with community groups that are under-represented in healthcare research. Our current projects also involve lay partner representatives as part of steering groups and project teams and sit on our iCARE Data Access Committee to ensure all research use of iCARE’s routine health data is of public and patient benefit.
Equality, Diversity and Inclusion
We will embed the EDI objectives by ensuring all new recruitments have a diverse interview panel and continuing to offer placements and apprenticeships, such as the HDRUK Black Internship Programme. We are also supporting Imperial College Healthcare NHS Trust to evaluate the effectiveness of their inclusive recruitment programme in increasing the ethnic diversity of senior roles within the Trust. Additionally, our diverse community partners will be invaluable in ensuring our research activities are inclusive and assess impacts on health inequalities. Finally, we are collaborating with local authorities, the voluntary sector, and Paddington Life Sciences industry partners to address digital exclusion in our Northwest London population.
Our Community Partners
In accordance with the Imperial BRC’s PPIEP Strategy , our theme has recruited a group of Community Partners to act as critical friends to our theme and share their valuable lived experience with our researchers and health professionals to help improve the relevance and quality of our research for the benefit of our North West London population.
Key Individuals
-
Erik Mayer
Director iCARE & Clinical Reader, Department of Surgery & Cancer -
Ana Luisa Neves
Advanced Research Fellow -
Ben Glampson
Senior Research Informatics Programme Manager -
Dr Aldo Faisal
Senior Lecturer in Neurotechnology -
Dr Bob Klaber
Director of strategy, research and innovation -
Professor Alessandra Russo
Head of Department of Computing -
Professor Azeem Majeed
Professor of Primary Care -
Professor Brendan Delaney
Chair in Medical Informatics and Decision Making -
Professor Deborah Ashby
Chair in Medical Statistics and Clinical Trials and Co-Director, ICTU -
Professor Mauricio Barahona
Chair in Biomathematics -
Professor Paul Aylin
Professor of Epidemiology and Public Health -
Professor The Lord Ara Darzi
Paul Hamlyn Chair of Surgery -
Professor Timothy Orchard
Professor of Gastroenterology -
Professor Victoria Cornelius
Director of Imperial Clinical Trials Unit -
Professor Wolfram Wiesemann
Head of Department of Analytics, Marketing & Operations