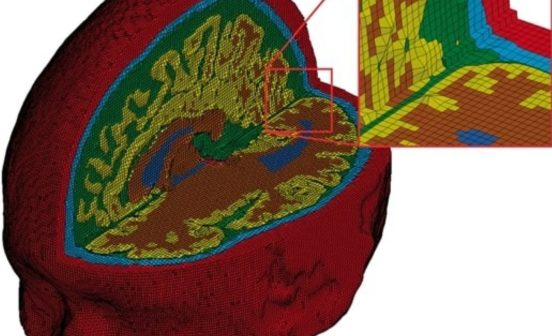
DiagnosticInformatics Approaches Artificial Intelligence (AI) improves stroke and dementia diagnosis in brain scans
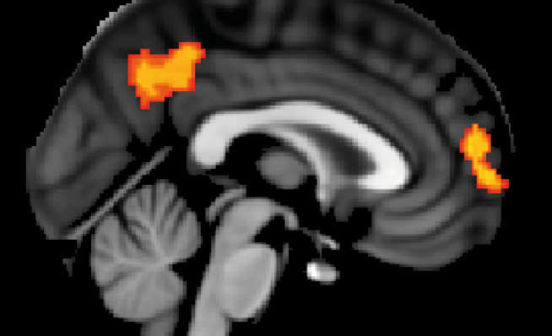
Scientists from the NIHR Imperial BRC, and from the University of Edinburgh have developed new software capable of detecting small vessel disease (SVD), a leading cause of stroke and vascular dementia.
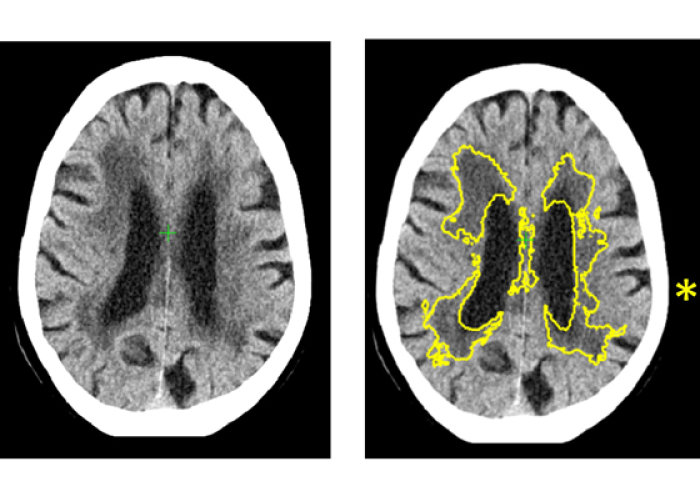
Currently, doctors diagnose SVD by looking for changes to white matter in the brain during MRI or CT scans. However, this relies on a doctor gauging from the scan how far the disease has spread, and it is often difficult to determine where the edges of the SVD are. Lead author, Dr Paul Bentley said “Current methods to diagnose the disease through CT or MRI scans can be effective, but it can be difficult for doctors to diagnose the severity of the disease by the human eye. The importance of our new method is that it allows for precise and automated measurement of the disease. This also has applications for widespread diagnosis and monitoring of dementia, as well as for emergency decision-making in stroke.”
The study, published in the journal Radiology, took place at Charing Cross Hospital, part of Imperial College Healthcare NHS Trust. It used historical data of 1082 CT scans of stroke patients across 70 hospitals in the UK between 2000-2014, including cases from the Third International Stroke Trial. The software identified and measured a marker of SVD, and then gave a score indicating how severe the disease was ranging from mild to severe. The researchers then compared the results to a panel of expert doctors who estimated SVD severity from the same scans. The level of agreement of the software with the experts was as good as agreements between one expert with another. In 60 cases they obtained MRI and CT in the same subjects and used the MRI to estimate the exact amount of SVD. This showed that the software is 85% accurate at predicting how severe SVD is.
Researchers say that this technology can help clinicians to administer the best treatment to patients more quickly in emergency settings, and predict a person’s likelihood of developing dementia. The development may also pave the way for more personalised medicine.
The study was funded by an NIHR i4i Invention for Innovation award, and an NIHR Imperial Biomedical Research Centre project grant. You can read the full story by Maxine Myers here.