DiagnosticInnovationPartnershipPrevention MRI tool can diagnose difficult cases of ovarian cancer
A new MRI tool has been developed that can identify cases of ovarian cancer which are difficult to diagnose using standard methods.
The tool is based on a 5-point scoring system of MRIs and has produced encouraging results that may help to identify the most appropriate treatment options. Its impact on the management and outcomes of women with ovarian cancer will now be evaluated in a major clinical trial at 18 hospitals in the UK, including Imperial College Healthcare NHS Trust.
The tool, developed by researchers led by Professor Isabelle Thomassin-Naggara at the APHP-Sorbonne Université, with Professor Andrea Rockall at Imperial College London, is able to distinguish between malignant and benign ovarian cysts with 90% accuracy, in cases that cannot be distinguished on ultrasound.
To investigate potential cases of ovarian cancer, doctors currently use ultrasound scanning and blood tests. However, in a quarter of cases these methods cannot identify with confidence whether a patient’s cyst is benign or malignant. This leads to surgical investigations, which are invasive and carry additional risks, such as potential loss of fertility. In most cases women are then diagnosed as having benign cysts.
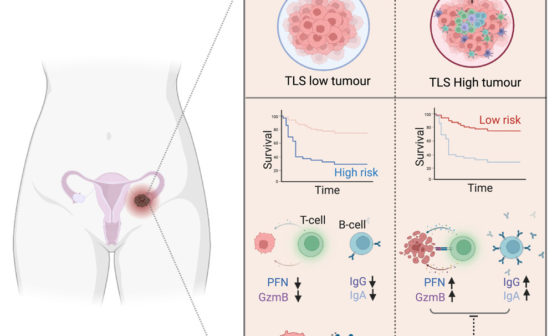
The team believes that the new tool can be used as a triage test to decide whether patients need further follow up or treatment. They also believe that findings from the study, published in the JAMA Network Open, could help stratify patients who are high risk so they can be given treatment at a much earlier stage.
Professor Andrea Rockall, Deputy Theme Lead of the NIHR Imperial BRC Imaging Theme and Chair of Radiology at Imperial College London, said:
“Ovarian cancer is referred to as a ‘silent killer’ as cases are often diagnosed at an advanced stage of the disease. When it is diagnosed earlier the chance of survival is much improved.
There is a real unmet clinical need to find less invasive ways to identify women at risk of ovarian cancer. Our tool has the potential to help triage patients who are low risk so they can have less invasive treatment options, as well as identifying high risk patients so they can receive treatment at an earlier stage and have a better chance of long-term survival.”
This research was funded Societé d’Imagerie de la Femme and supported by the NIHR Imperial BRC and Cancer Research UK Imperial Centre.
Read the full story by Maxine Myers, Imperial College London here.