Diagnostic AI stethoscope helping diagnose heart failure is rolled out to 100 GP clinics
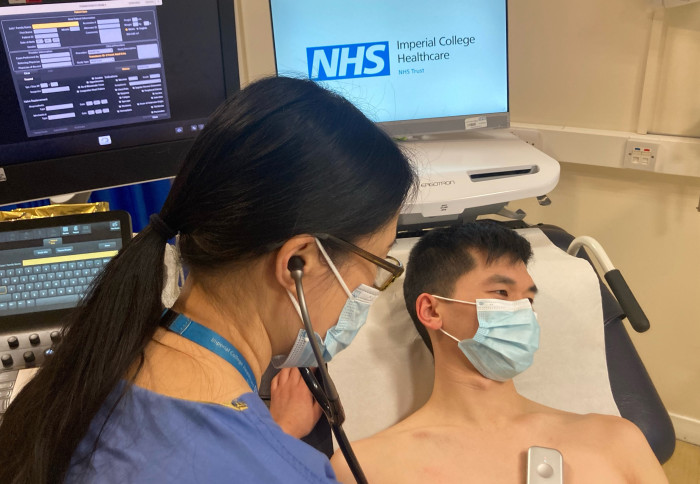
GP clinics in London and Wales will receive an AI-powered tool as part of a trial to help improve the diagnosis of a deadly heart condition. The TRICORDER programme led by researchers at Imperial College London and funded by a £1.2M Award from the NIHR will deploy AI-enabled smart stethoscopes to 100 primary care practices to assist clinicians in their evaluation of heart failure.
The original study, led by Professor Nicholas Peters, Professor of Cardiac Electrophysiology at the National Heart & Lung Institute and an NIHR Imperial BRC Cardiovascular Theme member, recruited over 1,000 NHS patients across seven sites in North West London, including Imperial College Healthcare NHS Trust (ICHNT) hospitals. The team found that combining a novel AI algorithm with a commercially available ‘smart’ stethoscope (Eko DUO) enabled them to provide an immediate diagnosis of heart failure with high levels of sensitivity and specificity (91% and 80%, respectively), compared to routine diagnostic tests that are invasive and expensive.
The project is believed to be the first of its kind, sector-wide use of an AI tool in primary care and will assess if the commercially available tool – the Eko DUO device – can improve diagnoses for heart failure and reduce costs for the NHS.
Heart failure is a condition in which the heart cannot pump blood effectively. It carries a higher risk of death than most cancers and is increasingly common, affecting 2% of the UK population and consuming 4% of the NHS budget.
Through the TRICORDER programme, researchers will now determine if providing GPs with the tool can increase early detection of heart failure for patients, reduce diagnosis through emergency hospital admission, and reduce costs for the NHS. Researchers believe that the widespread use of AI tools in primary care has the potential to improve heart disease outcomes for millions of people in the UK.
A total of 100 GP practices across Northwest London and North Wales, covering more than three million patients, will randomly be allocated to receive an AI-stethoscope or continue with usual care for patients.
Patients visiting their GP using the AI stethoscope will receive a brief, non-invasive heart exam, using an Eko digital stethoscope and app powered by the company’s AI. If the device detects possible signs of cardiac disease, the GP can rapidly start further tests and potentially life-saving treatments.
Patients continuing to attend GP clinics not using the AI tool will continue to receive typical care for detection and treatment of heart failure.
Professor Peters said: “Heart failure admission alone costs the UK over £2 billion annually, and an unacceptable 80% of these diagnoses are made during emergency admissions.”
Co-investigators Dr Patrik Bächtiger and Dr Mihir Kelshiker, from the National Heart and Lung Institute at Imperial, added: “TRICORDER is a system-wide implementation of Eko’s clinically effective AI technology. Implementing this tool in primary care could save the health payer system £2,400 per patient, eliminating the potential need for an emergency room visit.”
“Currently, four out of five patients are diagnosed too late, after emergency hospital admission, and they are likely to die prematurely. GPs have no accurate, easy-to-use tools to quickly check for heart failure. And if they suspect a patient may have heart failure, patients may go through a long and rarely completed pathway to diagnosis.
“Being able to diagnose heart failure early on maximises the benefits of treatments for patients, improving their symptoms, quality of life and survival.
The current gold standard for detecting heart failure is a blood test (NT-proBNP) that when ordered alone, can initiate a long pathway that may fail to achieve early diagnosis and treatment in those who need it most.”
Connor Landgraf, Co-founder and CEO of Eko Health, said: “This deployment around the UK of our AI-enabled heart disease detection technology demonstrates the need for accurate and early heart disease detection. We’re proud to partner with leading academic institutions such as Imperial College London to validate the clinical utility and positive impact our technology has on the lives of millions of patients.”
TRICORDER is a collaboration between The NHS Northwest London Integrated Care System, Betsi Cadwaladr University Health Board and Imperial College London.